Manual Muscle Testing in Functional Medicine: A Comprehensive Plan
Manual Muscle Testing (MMT) is a cornerstone of functional medicine, evaluating muscle function to identify imbalances linked to various physiological dysfunctions.
It assesses strength, revealing insights into neurological, nutritional, and hormonal health, guiding personalized treatment strategies for optimal wellness.
Manual Muscle Testing (MMT) is a foundational assessment technique within functional medicine, offering a non-invasive method to evaluate the strength and function of individual muscles. This process involves a clinician applying resistance while the patient attempts to contract specific muscle groups.
MMT isn’t merely about strength; it’s a window into the nervous system, nutritional status, and hormonal balance. Identifying weaknesses can pinpoint underlying imbalances, guiding targeted interventions for improved patient outcomes. It’s a crucial diagnostic tool.
The Core Principles of MMT

Core principles of MMT center around assessing voluntary muscle contraction against applied resistance. Accurate stabilization is paramount, isolating the targeted muscle and preventing compensatory movements. Consistent positioning ensures reliable results, and standardized grading – utilizing the 0-5 scale – provides objective measurement.
MMT acknowledges that muscle weakness isn’t always isolated; it often reflects systemic dysfunction. Therefore, a holistic approach, considering the interconnectedness of body systems, is essential for accurate interpretation.
MMT Grading Scale: A Detailed Breakdown
The MMT grading scale objectively quantifies muscle strength, ranging from 0 (no contraction) to 5 (normal strength against gravity and resistance). Grades 1-4 indicate varying degrees of weakness – partial range of motion, antigravity movement with assistance, or holding against slight/moderate pressure.
Precise observation of tendon prominence, contraction quality, and the ability to maintain a position are crucial for accurate grading, forming the basis for functional assessments.
Understanding the 0-5 Scale
The 0-5 MMT scale provides a standardized method for evaluating muscle strength. A grade of ‘0’ signifies no visible or palpable muscle contraction. ‘5’ represents normal strength – full range of motion against gravity with resistance. Intermediate grades (1-4) denote progressively improving strength,
with ‘1’ being a flicker of contraction and ‘4’ indicating good strength, but not normal. Accurate interpretation is vital for functional medicine assessments.
Specific Indicators for Each Grade (1-5)
Grade 1 shows a flicker of contraction, but no movement. Grade 2 allows movement through a partial range of motion. Grade 3 enables full range against gravity, but not with resistance. Grade 4 demonstrates good strength, yielding to moderate pressure.
Finally, Grade 5 signifies normal strength, sustaining a contraction through a full range of motion against maximal resistance, crucial for functional assessments.
Functional Medicine Perspective on Muscle Weakness
Functional Medicine views muscle weakness not as an isolated issue, but as a symptom reflecting underlying systemic dysfunction. It’s rarely a primary diagnosis. Investigating the root cause—such as gut health, nutrient deficiencies, or hormonal imbalances—is paramount.
Addressing these foundational issues, rather than solely targeting the muscle, is key to restoring optimal strength and overall wellbeing.
Muscle Weakness as a Symptom, Not a Diagnosis
In Functional Medicine, perceiving muscle weakness solely as a problem in the muscle is limiting. It’s a signal—a symptom—indicating a broader imbalance within the body’s interconnected systems;
Weakness prompts investigation into potential upstream causes like digestive issues, inflammation, or endocrine disruption, rather than simply prescribing muscle-focused exercises.
The Gut-Muscle Connection
A healthy gut profoundly impacts muscle function. Nutrient absorption, crucial for muscle repair and energy production, is heavily reliant on optimal gut health. Dysbiosis, or gut imbalance, can impair this process, leading to weakness.
Inflammation originating in the gut can also directly affect muscle tissue, hindering performance and recovery. MMT can help pinpoint these connections.
MMT Procedures: Step-by-Step Guide
Effective MMT requires a standardized approach. Begin with patient comfort and clear explanation. Proper positioning is vital – supine, prone, or seated – ensuring isolation of the target muscle.
Apply firm, steady pressure in the appropriate direction, observing for resistance. Note the grade based on observable movement and resistance levels, documenting findings accurately for comprehensive analysis.
Patient Positioning for Optimal Testing
Optimal MMT relies on precise patient positioning. Supine is ideal for hip flexion and extension, while prone suits plantarflexion. Sidelying facilitates abduction/adduction assessments.
Ensure the limb is stabilized proximally, isolating the target muscle. Comfort is key; adjust pillows as needed. Gravity’s role must be considered, adapting positions for weaker patients to gravity-eliminated planes.
Stabilization Techniques During MMT
Effective stabilization is crucial for accurate MMT. The examiner must firmly secure the origin of the muscle being tested, preventing unwanted compensatory movements.
Use a stable, comfortable grip, avoiding pressure on the joint itself. Proper stabilization isolates the target muscle, ensuring a reliable assessment of its strength and function, minimizing extraneous variables.
Key Muscle Groups to Assess in Functional Medicine
Functional MMT prioritizes assessing muscles impacting daily life. Key groups include trapezius (shoulder elevation), hip flexors, gluteals (hip extension), and ankle plantar flexors.
Upper and lower extremity testing reveals patterns of weakness. Evaluating these muscles provides insights into postural control, gait, and overall functional capacity, guiding targeted interventions.
Upper Extremity Muscle Testing
Upper extremity MMT focuses on shoulder abduction (trapezius), elbow flexion (biceps brachii), wrist extension (extensor carpi radialis), and grip strength (hand intrinsics).
Testing follows a preferred order, typically right then left, assessing each muscle’s ability to move through its range of motion against varying levels of resistance, revealing functional limitations.
Lower Extremity Muscle Testing
Lower extremity MMT evaluates hip flexion (iliopsoas), knee extension (quadriceps), ankle dorsiflexion (tibialis anterior), and plantarflexion (gastrocnemius/soleus).
The ankle plantar flexors are initially tested prone, then retested standing for accurate scoring. This systematic approach identifies weaknesses impacting gait, balance, and overall functional movement patterns, guiding targeted interventions.
MMT and Neuromuscular Dysfunction
MMT effectively identifies patterns of weakness suggesting neuromuscular issues. Specific weaknesses can pinpoint nerve impingement locations, impacting muscle function and movement.
Assessment extends to cranial nerve function, revealing deficits affecting facial expressions or swallowing. Recognizing these patterns allows functional medicine practitioners to address the root cause of dysfunction, not just symptoms.
Identifying Patterns of Weakness Related to Nerve Impingement
MMT reveals distinct weakness patterns indicative of nerve impingement. For example, weakness in specific shoulder muscles may suggest cervical nerve root compression.
Similarly, radicular pain accompanied by weakness in a myotomal distribution strongly suggests nerve involvement. Precise MMT helps localize the impingement, guiding targeted interventions like chiropractic adjustments or soft tissue mobilization.
MMT in Assessing Cranial Nerve Function
MMT extends beyond peripheral muscles to assess cranial nerve function. Evaluating facial muscle strength tests cranial nerve VII, identifying weaknesses from Bell’s palsy or stroke.
Testing tongue protrusion assesses hypoglossal nerve (XII) function, while assessing muscles of mastication evaluates trigeminal nerve (V). These assessments, combined with neurological exams, provide a comprehensive cranial nerve evaluation.
MMT for Nutritional Deficiencies

MMT reveals subtle muscle weaknesses indicative of underlying nutritional deficiencies. For example, reduced calf strength might suggest magnesium or potassium deficits. Generalized weakness can point to protein-calorie malnutrition or vitamin D insufficiency.
Specific muscle groups correlate with particular nutrient needs; monitoring MMT scores during nutritional interventions tracks the effectiveness of dietary changes and supplementation.
Correlation Between Specific Nutrient Deficiencies and Muscle Weakness
Specific nutrient deficits demonstrably impact muscle function, detectable via MMT. Potassium, calcium, and magnesium deficiencies often manifest as weakness in lower extremity muscles. Vitamin D insufficiency correlates with proximal muscle weakness, affecting shoulder and hip flexors.
Protein deficiency causes generalized weakness, while B vitamin deficiencies can lead to neurological symptoms alongside muscle fatigue and reduced strength.
Using MMT to Monitor Nutritional Interventions
MMT serves as an objective tool to track the efficacy of nutritional interventions. Baseline MMT assessments establish a starting point; subsequent testing quantifies improvements in muscle strength following dietary changes or supplementation.
Observable gains in MMT grades indicate successful nutrient repletion and improved muscle function, allowing for personalized adjustments to optimize patient outcomes and confirm treatment effectiveness.
MMT and Hormonal Imbalances
MMT can reveal subtle muscular weaknesses indicative of hormonal dysregulation. Thyroid dysfunction, for example, often presents as generalized muscle weakness, detectable through reduced MMT scores across multiple muscle groups.
Similarly, adrenal fatigue may manifest as diminished strength in antigravity muscles. Tracking MMT changes alongside hormone level adjustments provides valuable feedback on treatment progress and patient response.
Impact of Thyroid Dysfunction on Muscle Strength
Thyroid hormones are crucial for optimal muscle function; deficiencies lead to noticeable weakness. MMT frequently demonstrates reduced strength in proximal muscles – shoulder girdle, hip flexors – in hypothyroid patients.
Testing reveals diminished scores, particularly against gravity. Monitoring MMT scores during thyroid hormone replacement therapy helps assess treatment efficacy and guides dosage adjustments for improved muscular performance.

Assessing Muscle Weakness Related to Adrenal Fatigue

Adrenal fatigue often manifests as generalized muscle weakness, impacting endurance and recovery. MMT can reveal subtle declines in strength, especially during prolonged testing or later in the day, mirroring cortisol fluctuations.
Weakness may be more pronounced in antigravity muscles. Tracking MMT scores alongside adrenal support interventions provides valuable feedback on treatment progress and adrenal function restoration.
Integrating MMT with Other Functional Medicine Assessments
MMT’s true power lies in its integration with other functional medicine tools. Combining MMT findings with functional blood chemistry analysis provides a holistic view, correlating muscle weakness with specific nutrient deficiencies or hormonal imbalances.
This comprehensive approach allows for targeted interventions, maximizing therapeutic impact and ensuring a personalized, effective treatment plan for each patient’s unique needs.
Combining MMT with Functional Blood Chemistry Analysis
Integrating MMT with functional blood chemistry reveals crucial correlations. For example, consistent weakness in specific muscle groups, identified through MMT, may align with low levels of vitamin D, magnesium, or potassium on blood tests.
This synergy allows practitioners to pinpoint underlying biochemical imbalances driving muscle dysfunction, leading to more precise and effective nutritional interventions.
MMT as Part of a Comprehensive Functional Assessment

Manual Muscle Testing shouldn’t exist in isolation; it’s most powerful within a broader functional assessment. This includes detailed patient history, symptom analysis, and advanced lab testing.
MMT findings, combined with gut health evaluations, hormone panels, and neurological assessments, create a holistic picture, revealing interconnectedness and guiding truly personalized treatment plans.
Common Errors in MMT and How to Avoid Them
Inconsistent stabilization is a frequent MMT error; maintain firm, neutral support throughout testing. Incorrect patient positioning also impacts results – ensure proper alignment for accurate assessment.
Variability in pressure application and failing to test bilaterally can skew findings. Standardized procedures, meticulous technique, and ongoing practice are crucial for reliable MMT outcomes.
Inconsistent Stabilization Techniques
Inconsistent stabilization during MMT compromises accuracy; the tester must provide firm, neutral support, isolating the targeted muscle. Varying pressure or position alters the test, yielding unreliable results.

Proper stabilization prevents compensatory movements, ensuring the assessed muscle performs the action independently. Consistent technique requires practice and awareness of body mechanics for valid assessments.
Incorrect Patient Positioning
Incorrect patient positioning significantly impacts MMT results, hindering accurate muscle assessment. Proper alignment ensures the muscle’s line of pull is optimal for testing, minimizing extraneous strain.
Failure to position correctly can lead to false weakness readings or mask true deficits. Standardized positions – prone, supine, sitting – are crucial for reliable, repeatable evaluations and effective functional medicine interventions.
MMT in Pediatric Functional Medicine
Manual Muscle Testing (MMT) in pediatrics requires age-specific adaptations due to developmental variations. Assessing muscle strength helps identify developmental delays and neurological concerns early on.
Functional medicine practitioners utilize MMT to evaluate muscle function, considering a child’s evolving motor skills and growth patterns, tailoring interventions to support optimal development and address underlying imbalances.
Age-Specific Considerations for MMT in Children
MMT protocols must be modified based on a child’s age and developmental stage. Infants require passive movement assessment, while toddlers benefit from play-based testing.
Older children can participate in traditional MMT, but grading scales should account for age-related strength norms. Practitioners must consider a child’s cognitive and emotional maturity for accurate and reliable results.
Identifying Developmental Delays Through MMT
MMT can reveal subtle muscle weakness patterns indicative of developmental delays in children. Assessing muscle strength against gravity helps pinpoint areas where a child isn’t meeting expected milestones.
Consistent weakness in specific muscle groups may signal neurological or musculoskeletal issues impacting gross motor skills. Early detection through MMT facilitates timely intervention and improved outcomes.
Advanced MMT Techniques
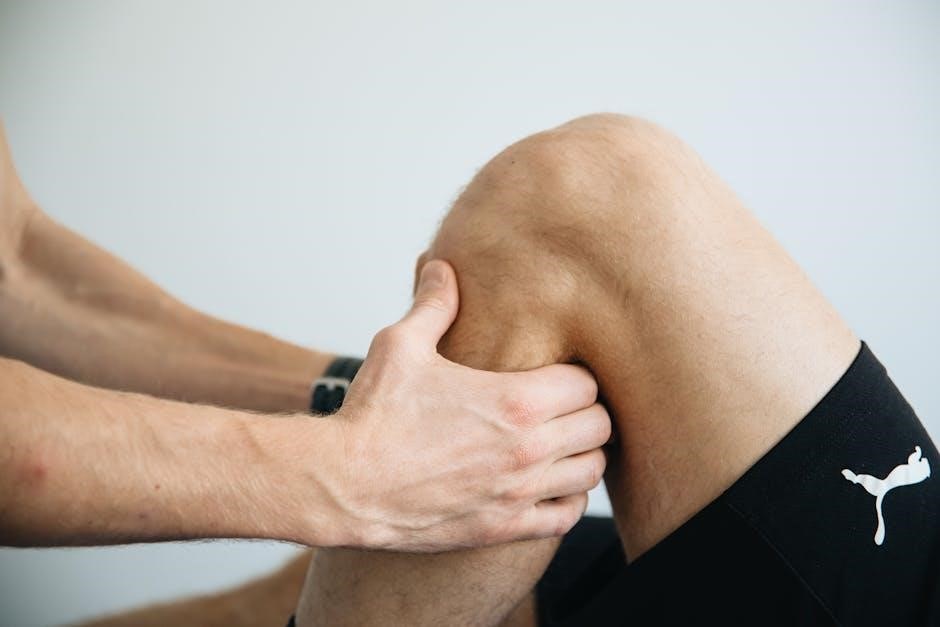
Beyond standard testing, advanced techniques refine functional assessments. Resisted Range of Motion (RROM) evaluates strength throughout the entire movement arc, identifying specific weak points.
Dynamic Palpation during MMT assesses muscle tissue quality, detecting subtle changes in tone or tenderness. These methods provide a more nuanced understanding of neuromuscular function, enhancing diagnostic accuracy.
Resisted Range of Motion Testing
Resisted Range of Motion (RROM) assesses muscular strength dynamically throughout a movement’s full arc. The examiner applies gentle, opposing force while the patient performs the motion.
This technique pinpoints specific weaknesses, unlike standard MMT which evaluates endpoint strength. RROM identifies functional limitations and guides targeted interventions, improving rehabilitation outcomes and functional capacity.
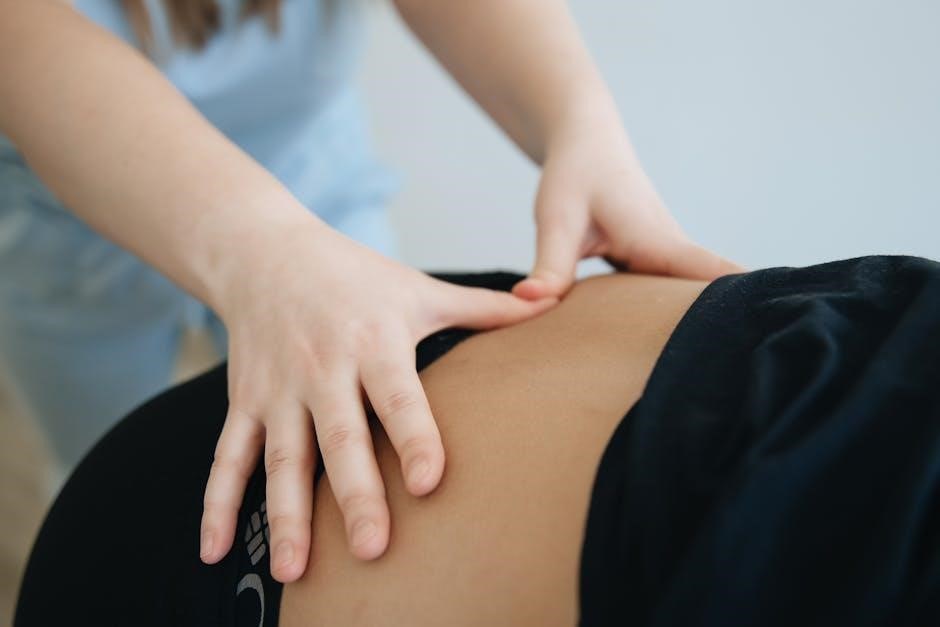
Dynamic Palpation During MMT
Dynamic Palpation enhances MMT by assessing muscle tissue quality during contraction. The examiner feels for changes in muscle tone, tenderness, or fascial restrictions as the patient moves.

This reveals subtle dysfunction not detectable by strength grading alone, identifying trigger points or areas of altered tissue texture. It refines assessment, informing targeted soft tissue work and improving treatment precision.
Documentation and Interpretation of MMT Findings
Detailed documentation of MMT results is crucial, including grade, any observed compensations, and qualitative findings like pain or fatigue.
Interpretation requires correlating muscle weakness patterns with patient history and other functional assessments. A clear report facilitates tracking progress and adjusting interventions, ensuring a holistic and personalized approach to care.
Creating a Clear and Concise MMT Report
An effective MMT report should systematically list tested muscle groups, their corresponding grades (0-5), and any observed deviations from normal movement.
Include details on stabilization techniques used and patient positioning. Concise language and objective observations are key, avoiding subjective interpretations. This structured format ensures accurate communication and facilitates collaborative care.
Interpreting MMT Results in the Context of the Patient’s History
MMT findings gain significance when correlated with a patient’s comprehensive history – symptoms, diet, lifestyle, and relevant medical conditions.
Weakness patterns can suggest underlying issues like nutritional deficiencies or hormonal imbalances. Consider the timing of weakness onset and any exacerbating factors. This holistic approach ensures MMT informs targeted functional medicine interventions.
The Future of MMT in Functional Medicine
The future of MMT lies in technological integration, potentially utilizing digital dynamometers for objective strength measurements and enhanced data analysis.
Expanding MMT’s role in personalized medicine involves refining pattern recognition and linking findings to genetic predispositions. This will allow for more precise, individualized treatment plans, optimizing patient outcomes and preventative care strategies.
Technological Advancements in MMT
Emerging technologies are poised to refine MMT, moving beyond subjective assessment. Digital dynamometers offer quantifiable strength data, reducing inter-rater variability and improving precision.
Software integration can analyze muscle patterns, correlating them with functional limitations and aiding in targeted rehabilitation. These advancements promise more objective, data-driven insights into muscle function and overall health.
Expanding the Role of MMT in Personalized Medicine
MMT’s future lies in its integration with comprehensive patient data, fueling truly personalized treatment plans. By combining MMT findings with genetic predispositions, microbiome analysis, and metabolic assessments, clinicians can pinpoint root causes of dysfunction.
This holistic approach allows for tailored interventions—nutritional adjustments, targeted exercise, and lifestyle modifications—optimizing individual health outcomes.



